Step 1 Completing a Medicaid Application
Not sure if you qualify? Apply to find out.
IMPORTANT:
- If you do not choose a health plan, one will be chosen for you. Visit Choose a Plan for more information about selecting a plan.
- When applying online, make sure you:
- Check the box showing the child has a disability on the Additional Personal Details screen:

- Select the child and choose “Disabled” from the list:
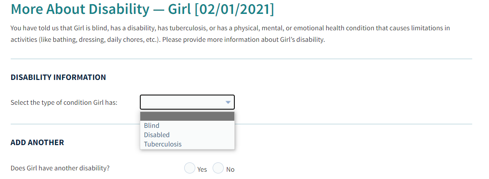
- Check the box showing the child has a disability on the Additional Personal Details screen:
- If you apply using a paper application, answer “yes” to the disability question (as shown in question 12 below) so your application is reviewed for Act 421-CMO:

 Official Louisiana State Websites use .la.gov
Official Louisiana State Websites use .la.gov  Secure .gov websites use HTTPS
Secure .gov websites use HTTPS 